Acute Pancreatitis
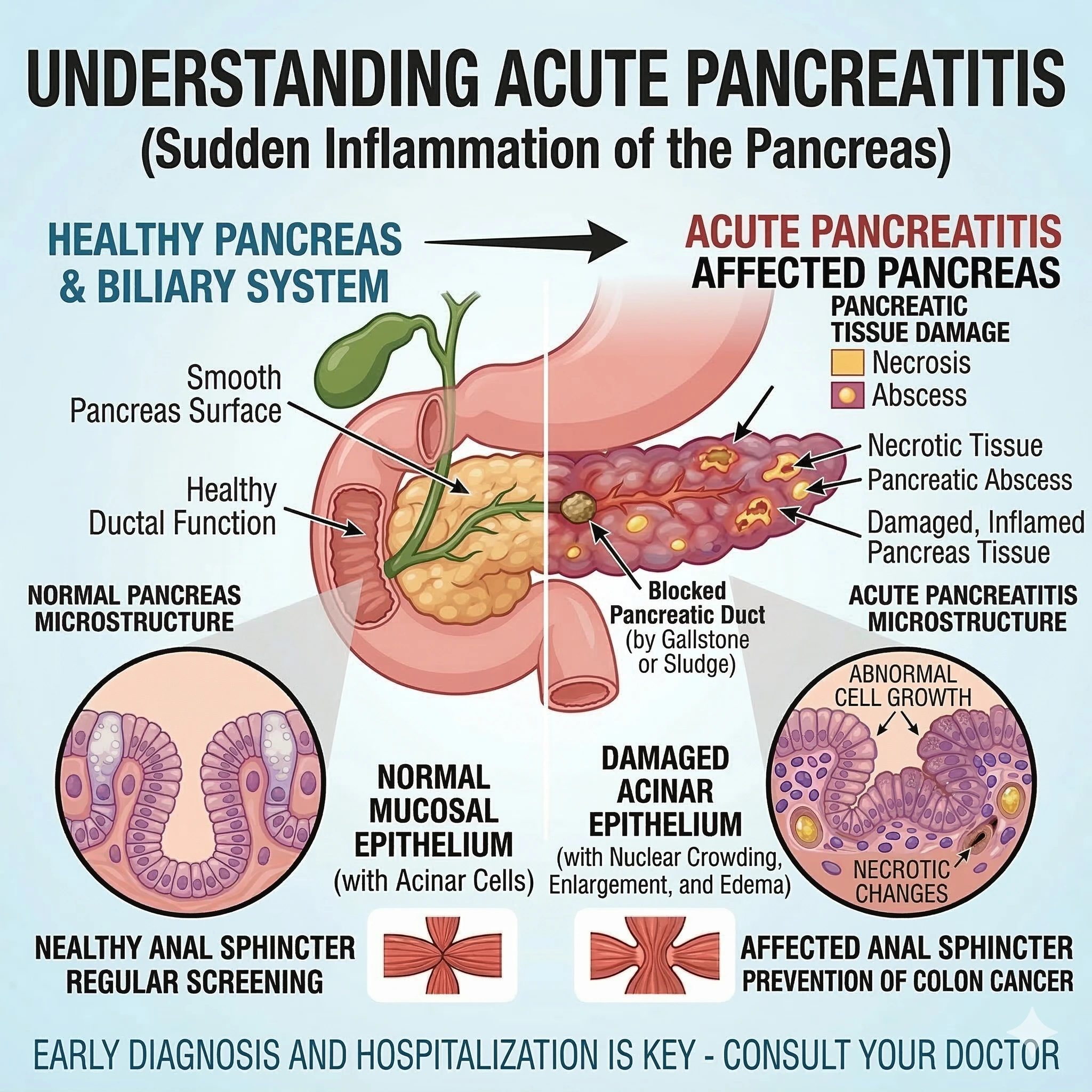
Acute pancreatitis is a sudden inflammation of the pancreas, a gland located behind the stomach that helps the body digest food and regulate blood sugar.
During acute pancreatitis, digestive enzymes become activated inside the pancreas instead of the small intestine. This causes the pancreas to become inflamed and irritated, leading to severe abdominal pain and digestive symptoms.
Acute pancreatitis can range from mild inflammation that resolves with treatment to a more serious condition requiring hospitalization. With early diagnosis and proper medical care, most people recover completely.
Common Symptoms to Watch For
• Severe pain in the upper abdomen
• Pain that may spread to the back
• Nausea and vomiting
• Abdominal tenderness or swelling
• Fever
• Rapid pulse
• Loss of appetite
• Indigestion or bloating
How is Acute Pancreatitis Diagnosed?
Doctors diagnose acute pancreatitis through a combination of clinical symptoms, blood tests, and imaging studies.
Blood Tests
Blood tests are used to measure pancreatic enzymes such as amylase and lipase, which often become elevated during pancreatitis.
Ultrasound
An abdominal ultrasound may be performed to check for gallstones or bile duct blockage.
CT Scan
A CT scan provides detailed images of the pancreas and helps assess the severity of inflammation.
MRI or MRCP
These imaging tests help evaluate the pancreatic ducts and surrounding organs.
Acute Pancreatitis treatment at Lifeline Clinic
Comprehensive Evaluation
Accurate Diagnosis
Personalized Treatment
Treatment for Acute Pancreatitis
Treatment focuses on reducing inflammation and allowing the pancreas to heal.
Hospital Care
Most patients with acute pancreatitis require hospital monitoring.
Treatment may include:
• Intravenous fluids to prevent dehydration
• Pain management
• Temporary fasting to allow the pancreas to rest
• Nutritional support if required
Treating the Underlying Cause
If gallstones are responsible, doctors may recommend gallbladder removal surgery after recovery.
If alcohol is the cause, avoiding alcohol completely is important to prevent recurrence.
Possible Complications
Although many cases are mild, severe pancreatitis may lead to complications such as:
• Pancreatic infection
• Fluid collections or pseudocysts
• Breathing problems
• Kidney problems
• Digestive difficulties
Early treatment significantly reduces the risk of complications.
When to seek medical help?
• Severe upper abdominal pain
• Persistent vomiting
• Fever along with abdominal pain
• Pain spreading to the back
• Difficulty eating or drinking
Related Images
Other Conditions
Frequently Asked Questions
I have severe pain in the upper abdomen that goes to my back. Could this be pancreatitis?
Pain that starts in the upper abdomen and radiates to the back is a common symptom of pancreatitis. However, other digestive conditions can also cause similar symptoms, so medical evaluation is necessary.
Can acute pancreatitis go away on its own?
Mild cases may improve with supportive treatment such as fluids and rest for the pancreas. However, medical supervision is important to prevent complications.
How long does acute pancreatitis last?
Mild acute pancreatitis usually improves within a few days to a week, while more severe cases may take longer to recover.
Is acute pancreatitis life-threatening?
Most cases are mild and recover well with treatment, but severe pancreatitis can be serious and requires hospitalization.

