Chronic Pancreatitis
Chronic pancreatitis is a long-term inflammation of the pancreas, the organ located behind the stomach that helps digest food and regulate blood sugar.
Unlike acute pancreatitis, which occurs suddenly, chronic pancreatitis develops gradually over time and leads to permanent damage to the pancreas. As the inflammation continues, the pancreas slowly loses its ability to produce digestive enzymes and hormones.
This can result in persistent abdominal pain, difficulty digesting food, weight loss, and sometimes diabetes.
Early diagnosis and proper treatment can help manage symptoms and prevent further damage.
Common Symptoms to Watch For
• Persistent upper abdominal pain
• Pain that spreads to the back
• Pain that worsens after eating
• Nausea or vomiting
• Unexplained weight loss
• Oily or greasy stools (steatorrhea)
• Diarrhea
• Loss of appetite
• Fatigue
• Development of diabetes
How is Chronic Pancreatitis Diagnosed?
Diagnosing chronic pancreatitis may require several tests.
Blood Tests
Blood tests may evaluate pancreatic enzyme levels and check for nutritional deficiencies.
CT Scan
A CT scan provides detailed images of the pancreas and can detect inflammation, calcification, or structural changes.
MRI or MRCP
These imaging tests evaluate the pancreatic ducts and surrounding structures.
Endoscopic Ultrasound (EUS)
EUS allows doctors to obtain highly detailed images of the pancreas and detect early changes.
Stool Tests
These tests may help determine whether the pancreas is producing enough digestive enzymes.
Chronic Pancreatitis treatment at Lifeline Clinic
Comprehensive Evaluation
Accurate Diagnosis
Personalized Treatment
Treatment for Chronic Pancreatitis
Pain Management
Medications and lifestyle changes may help control chronic abdominal pain.
Pancreatic Enzyme Supplements
Patients may require enzyme supplements to help digest food properly.
Dietary Modifications
A low-fat diet and smaller, more frequent meals may reduce pancreatic stress.
Treatment of Underlying Causes
If alcohol or smoking is contributing to the condition, stopping these habits is essential.
Endoscopic or Surgical Treatment
In certain cases, procedures may be required to remove blockages or improve pancreatic drainage.
When to seek medical help?
• Persistent upper abdominal pain
• Pain that spreads to the back
• Oily or greasy stools
• Unexplained weight loss
• Frequent digestive problems
• Symptoms of diabetes
Related Images
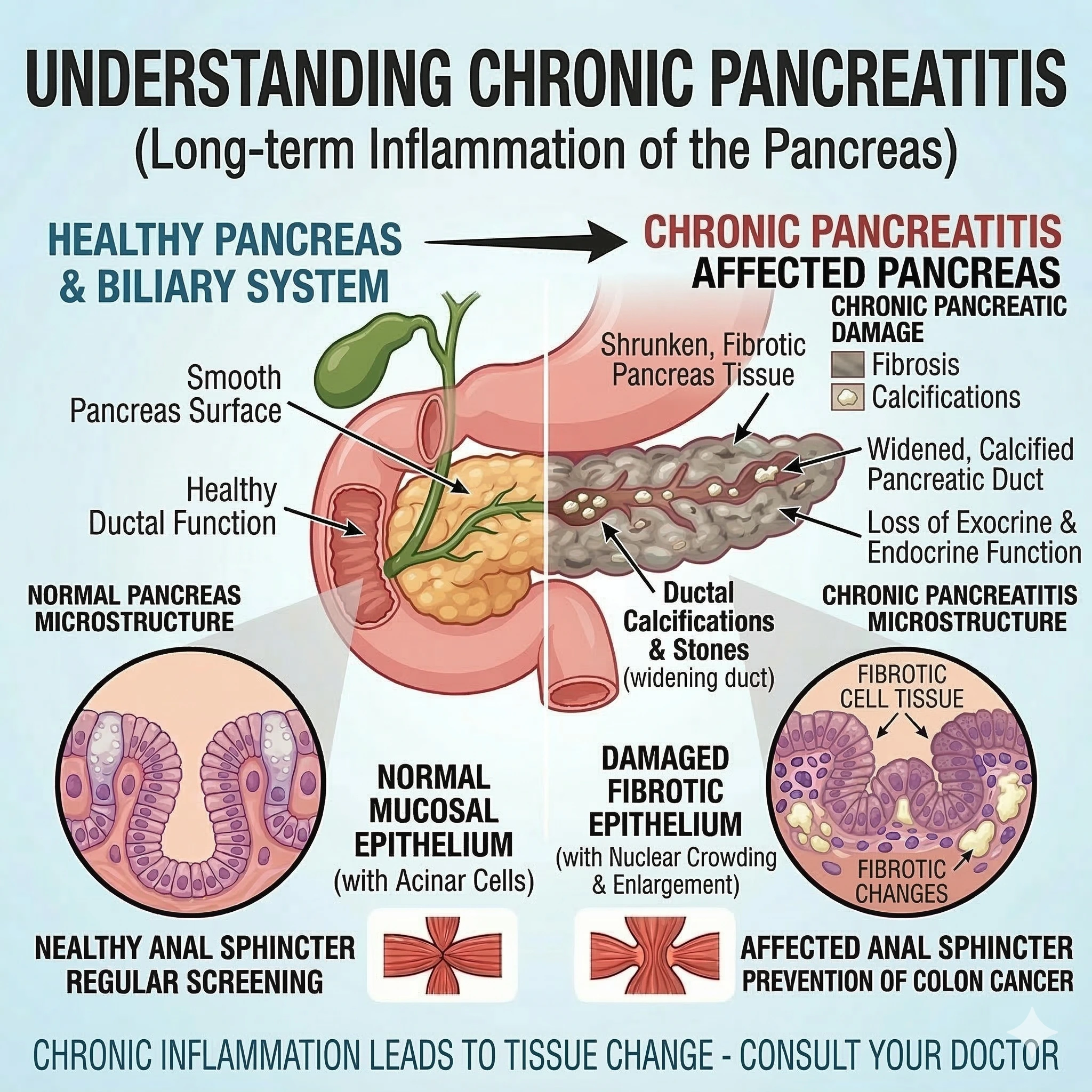
Other Conditions
Frequently Asked Questions
I have long-term pain in my upper abdomen that goes to my back. Could this be chronic pancreatitis?
Persistent upper abdominal pain that spreads to the back can be a symptom of chronic pancreatitis. However, similar symptoms can occur in other digestive conditions, so medical evaluation is necessary.
Why do I have oily or floating stools?
Oily or floating stools may occur when the pancreas does not produce enough digestive enzymes. This condition, known as pancreatic insufficiency, is common in chronic pancreatitis.
I am losing weight even though I am eating normally. Could this be chronic pancreatitis?
Unexplained weight loss can occur in chronic pancreatitis because the body may not properly digest and absorb nutrients from food. When the pancreas cannot produce enough enzymes, digestion becomes less efficient.
Can chronic pancreatitis happen without drinking alcohol?
Yes. Although alcohol is a common cause, chronic pancreatitis can also occur due to genetic factors, autoimmune diseases, repeated acute pancreatitis attacks, high triglyceride levels, or structural abnormalities of the pancreas.

